Catatonia is a fascinating medical condition marked by changes in muscle tone or activity associated with a large number of serious mental and physical illnesses. It was described for the first time by a German psychiatrist, Karl Ludwig Kahlbaum in 1874. The exact mechanisms underlying the pathophysiology of catatonia still remain a mystery. It seems that some people are more predisposed than others to develop this syndrome.
You might have seen this condition in some movies where the actor/patient seems to not respond to anyone or anything around him, being lost in his world and losing contact with reality. The best representation of this condition, I think, could be found in the movie Awakenings (1990) with Robert De Niro and Robin Williams.
The origin of the word Catatonia was traced back to late 19th century and it arrived from the combination of “cata” meaning badly and “tonos” meaning tension or muscular tone, therefore it can be loosely translated as “bad muscular tone”.
There are two distinct sets of symptoms that are characteristic of this condition.
In catatonic stupor (lethargy) motor activity may be reduced to zero. Individuals avoid bathing and grooming, make little or no eye contact with others, may be mute and rigid, and initiate no social behaviors. For example, the patient sits immobile in a chair for sixteen hours, staring fixedly, apparently unaware of other people or his own bodily needs. Specific to this condition is also a behavior known as cerea flexibilitas (waxy flexibility) in which the individual can be made to assume bizarre (and sometimes painful) postures that they will maintain for extended periods of time without no apparent fatigue or effort. The individual may become dehydrated and malnourished because food and liquids are refused. In extreme situations such individuals must be fed through a tube. This is the most common type of catatonia.
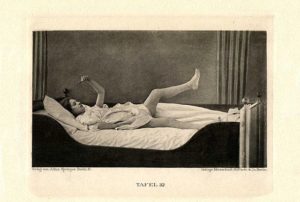
Cerea flexibilitas
Catatonic excitement is characterized by hyperactivity and violence; the individual may harm him/herself or others. On rare occasions, isolation or restraint may be needed to ensure the individual’s safety and the safety of others.
Catatonia can also be categorized as intrinsic or extrinsic. If the condition has an identifiable cause, it is designated as extrinsic. If no cause can be determined following physical examination, laboratory testing, and history taking, the illness is considered to be intrinsic.
In terms of the most common associated signs with this rare condition, in a study involving more than 230 catatonic patients, the “staring,” was found in more than 80% of cases. Among other frequent signs, were the immobility in 70% of cases, the mutism (refusing to speak) in 60% of patients, and the withdrawal in 50% of them.
The causes of catatonia are largely unknown although research indicates that brain structure and function are somehow altered in this condition. While this and other information point to a physical cause, none has yet been proven. A variety of medical conditions also may lead to catatonia including head trauma, cerebrovascular disease, encephalitis, and certain metabolic disorders.
Catatonia was linked for a long time exclusively with schizophrenia. However, recent epidemiological studies showed that schizophrenia is found only in 20% of catatonic cases while mood disorders underlie 45% of cases. Catatonia is also frequent in children and adolescents, particularly in autism spectrum disorders where the prevalence varies between 12 and 17%.
Features of catatonia may also be seen in Neuroleptic Malignant Syndrome (NMS) which is an uncommon (but potentially lethal) reaction to some medications (antipsychotics) used to treat major mental illnesses. It will appear within 10 days of starting the drug in 90% of the cases. NMS is considered a medical emergency since 25% of untreated cases result in death.
It is estimated that approximately 90,000 cases of catatonia occur each year in US hospitals. Catatonia has a reported prevalence ranging from 7.6 percent to as high as 38 percent in psychiatric patients. It is most commonly associated with mood disorders (depression, bipolar disorders).
There are no laboratory or other tests that can be used to positively diagnose this condition, but medical and neurological tests are necessary to rule out underlying lesions or disorders that may be causing the symptoms observed.
Treatment of catatonia includes medications such as benzodiazepines (Xanax, Valium, Ativan etc) which are the first line of treatment. Electroconvulsive therapy (ECT) is most effective treatment for catatonic depression and may prove beneficial for clients who do not respond to medication. If these approaches are unsuccessful, treatment will be redirected to attempts to control the signs and symptoms of the illness.
There is currently no known way to prevent catatonia because the cause has not yet been identified. Research efforts continue to explore possible origins. Avoiding excessive use of neuroleptic (antipsychotic) drugs can help minimize the risk of developing catatonic-like symptoms.
Various drugs
And finally, there is interesting medical research that considered catatonia as an evolutionary remainder of defense strategies associated with intense fear. It seems that in front of predators, several survival behaviors have been developed. Among them, the most known one was the “fight or flight” strategy. In cases where none of these two options was possible, a third strategy called “tonic immobility” (TI) would be set up which consists of a tonic suspension of motor activity. This defense strategy is based on the fact that many predators are attracted by their prey’s movements. This hypothesis seems to be confirmed by the subjective experience of catatonic patients. Indeed, once remitted from their catatonia, patients report having felt invaded by a major and uncontrollable anxiety. Conversely, they do not seem to have been aware of their motor state and the time lapsed.
